Case Study Spotlight: Mary’s Center
Why Proving Community Health Solutions Requires More Than Results
For 38 years, Mary's Center in Washington, DC, has served thousands of participants through an integrated model merging medical care, education, and social services, ranking among the top federally qualified health centers nationwide. In 2019, the Urban Institute validated its approach through a comprehensive year-long study, but five years later, Mary's Center still lacks the resources to demonstrate long-term cost-effectiveness, identify which components drive results, or adapt its model for different communities. Community health organizations across the country face the same challenge: innovating and getting results without research infrastructure to document what works, share lessons, or build evidence for sustainable funding. Each starts from scratch, proving to individual funders what others have already proven.
The National Hispanic Health Research Institute exists to connect grassroots health providers with the research institutions, funding, and training needed to turn community knowledge into collective evidence. We help organizations access multi-year research partnerships, build evaluation capacity, and create networks for shared learning. The solutions already exist in communities. What's missing is investment in the research infrastructure to validate, refine, and spread what works.
Here’s Mary’s Center’s story:
The Problem: Success Without the Science to Spread It
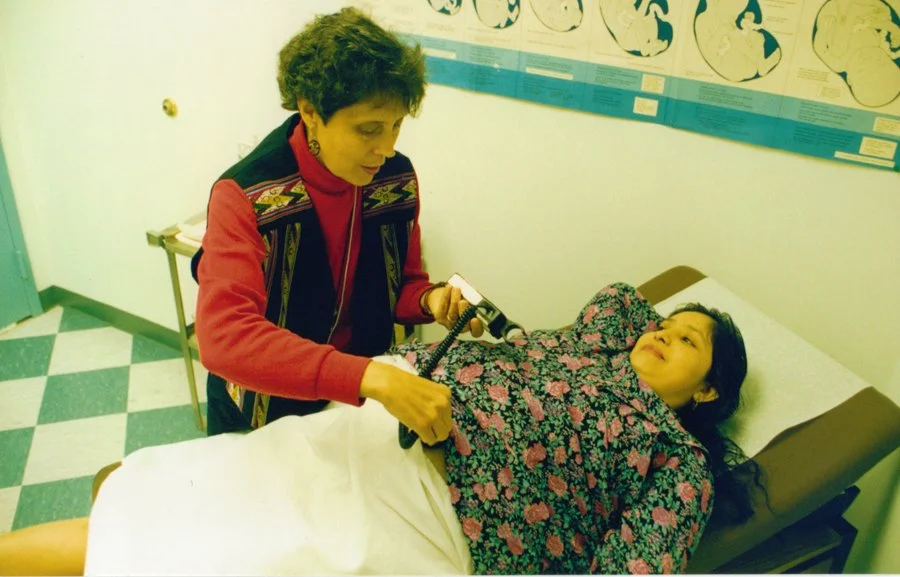
When nurse Maria Gomez opened a prenatal clinic in a Washington, D.C. rowhouse basement in 1988, she was fulfilling a need. Central American women fleeing civil wars needed help navigating a new country and a new system. They also needed medical care.
Photo Credit: Mary’s CenterShe set up a clinic that offered prenatal and pediatric care, and gradually expanded its programs as additional needs were identified. Ten years later, Mary’s Center added services and became a place where participants learned English, found housing, and could raise their children in a place that felt a bit more like home.
Almost four decades later, Mary's Center serves over 65,000 people annually across five locations. They rank among the best federally qualified health centers in the country. Their national recognition as a health center quality leader by the Health Resources and Services Administration (HRSA), a division of the US Department of Health, has yielded positive results for patients too. Over the years, it has been demonstrated that using multiple services has helped lower rates of diabetes, hypertension, and obesity compared to those receiving medical care alone.
But without peer-reviewed studies, cost-effectiveness analyses, and multi-site trials, Mary's Center couldn't answer the questions that would enable other communities to reproduce its success.
In 2019, they partnered with the Urban Institute for a comprehensive evaluation.
What researchers soon found out was that Mary’s Center’s culture and program integration were the most relevant factors in making a difference for participants.
Staff described the organization as mission-driven and demanding, where people performed "at the top of their license." When hiring anyone from a director to a front desk person, leadership led with the mission in mind. "Your longevity here depends on whether you believe in what we are doing here," one staff member explained.
Mary's Center set a goal that included that 70 percent of staff should reflect the race and ethnicity of the patients they serve. By 2018, 56 percent of staff identified as Hispanic, 15 percent as Black or African American. Among senior leadership, 44 percent were people of color compared to just 17 percent at hospitals nationally.
The Washington Post has named Mary's Center one of the top workplaces in the metropolitan area on five occasions: Ninety percent of staff reported being enthusiastic and passionate about their work, compared to just 32 percent of all U.S. employees.
But the real innovation was in the details of their care and attention to the participants. In the Urban Institute report, staff called it "warm handoffs." Instead of giving patients a referral slip and hoping they'd follow up, providers walked them directly to their next appointment. For people with busy lives, transportation challenges, and wariness of medical systems, that simple act dramatically increased the likelihood they'd get the care they needed.
"We think it's really important not just to say, 'I'll make another appointment for you with a family support worker,'" one staff member explained. "Instead, you go and introduce the person to the provider to remove that barrier."
Electronic medical records supported those handoffs. When a pediatrician saw a child with asthma, they could see that the parent was dealing with depression, enrolled in workforce training, and receiving support from a home visiting nurse. Staff across departments could coordinate care seamlessly.
The combination of high-tech systems and high-touch personal connections was what staff called their "secret sauce."
Researchers spent a year documenting everything. They surveyed 300 staff members, interviewed 35 patients and 14 community partners, and analyzed decades of medical records. They worked with the National Institutes of Health and the University of Maryland.
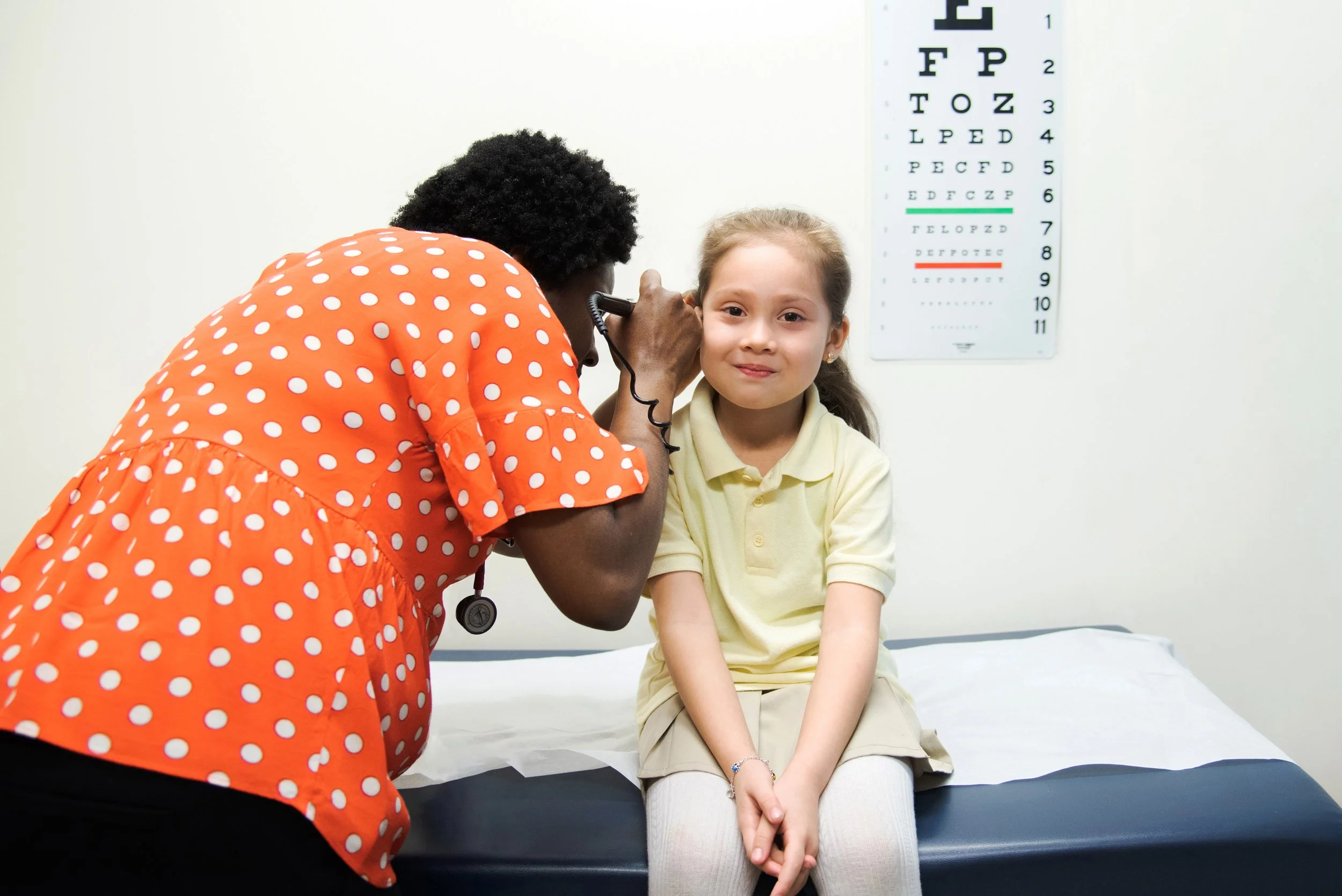
Photo Credit: Mary's Center
The findings validated what Mary's Center already knew. The model worked because of mission-driven staff, warm handoffs, coordinated services, and continuous quality improvement.
When Mary's Center partnered with George Washington University in 2015 to assess patient satisfaction, 98 percent said they would recommend the center to a friend. But surveys also revealed long wait times. Mary's Center responded by contracting with an off-site call center, reducing dropped calls from 20 percent to less than 5 percent. They redesigned clinic layouts and triage procedures, reducing the maximum wait time from 45 to 15 minutes.
The Urban Institute concluded: "Mary's Center provides a useful framework for understanding the benefits of comprehensive medical, social, and educational services in under-resourced communities."
Then they identified a shortcoming in duplicating this model.
The study examined one organization in one city serving primarily one population. What about rural communities? Different cultural contexts? Multi-generational families?
Did patients who used multiple services have better outcomes because of integrated care, or were they already more stable? How much did each component contribute? What's the cost-effectiveness compared to traditional care?
The analysis compared participants who received both primary care and other services to those who received only medical care. Results showed a lower risk of chronic disease among those using multiple services. But researchers couldn't control all the factors that might explain those results. Households accessing more services might be more vulnerable, or they might be more stable and therefore able to take advantage of offerings.
"More work is needed to articulate how social change model services impact individual and family health," the researchers wrote. "This will require additional resources to support data management and research."
Five years later, that work hasn't happened.
Larger problem
Federally qualified health centers serve over 30 million Americans, mostly low-income, uninsured, or publicly insured. Many are developing creative approaches to integrated care, hiring community health workers, and confronting social determinants of health.
They're doing it without research infrastructure. No evaluation staff. No data systems beyond billing. No partnerships with research institutions. No time for staff to participate in studies.
Each organization starts from scratch, proving to individual funders what others have already proven. Reinventing approaches that could be shared. Generating local knowledge that never becomes collective evidence.
Why NHHRI Exists
The National Hispanic Health Research Institute was created to solve this problem. We connect grassroots health providers with research institutions that can partner on rigorous evaluation. We help organizations access funding for multi-year studies. We provide training in research methods that respect community knowledge. We create networks so innovations in one community can inform practice in others.
The 2019 Urban Institute study showed what's possible when a community health center partners with researchers for an extensive evaluation. We're working to make that level of research support accessible to organizations nationwide.
What Sustained Research Could Accomplish
With investment into research infrastructure, community health organizations could track multi-generational impacts. Answers to important questions like: Do the children of participants have better health outcomes? Do educational programs change economic directions over decades? And, most importantly, is this a financially sustainable model?
To compare approaches across different scenarios, more questions need to be researched.
Right now, community health organizations are addressing social determinants of health without the resources to demonstrate impact. The inability to get results without data to demonstrate cost-effectiveness put everyone at a disadvantage. Innovating without sharing lessons costs providers across the country time and money, including the inability to access funding from donors who increasingly call for rigorous evidence to move forward.
NHHRI exists to help community health providers build the evidence base that can inform practice and policy throughout diverse communities.
We need funding for the research that can turn community knowledge into collective evidence, and collective evidence into transformed systems of care. And we need it now before the model is discarded and lost to the pages of history.
About Mary’s Center:
Founded in 1988, Mary’s Center is a community health center that provides healthcare, educational, and social services to more than 65,000 individuals from over 50 countries. Using a holistic, multipronged approach, Mary’s Center helps each participant access individualized services that set them on the path toward good health, stability, and economic independence. For more information, visit www.maryscenter.org.
About NHHRI:
The National Hispanic Health Research Institute connects community health providers with research institutions, funding sources, and training to document impact and share solutions.